Ingrown Toenail Care
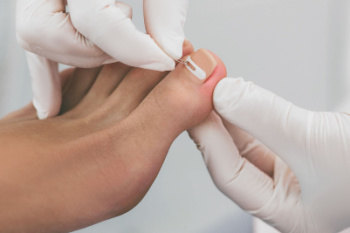
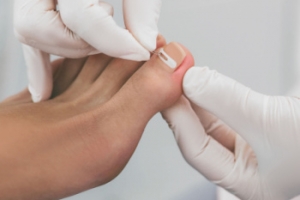
Ingrown toenails occur when the edges of a toenail grow into the surrounding skin, causing pain, redness, and swelling. This condition is often seen in the big toe and can sometimes lead to infection. One of the key causes of ingrown toenails is improper nail trimming, such as cutting nails too short or rounding the edges. Other factors include wearing tight shoes that crowd the toes or injure the nail. Toenail thickening, often caused by fungal infections, can also increase the risk of ingrown nails by altering the shape of the nail and making it more likely to dig into the skin. Ingrown toenails may improve with care like soaking and proper trimming, but severe cases require professional treatment. A podiatrist can safely remove part of the nail, treat any infection, and provide advice on proper nail care and footwear to prevent recurrence. If you have an ingrown toenail, it is suggested that you schedule an appointment with a podiatrist.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact Priyanka Mude, DPM of North Canton Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
- Improper toenail trimming
- Genetics
- Improper shoe fitting
- Injury from pedicures or nail picking
- Abnormal gait
- Poor hygiene
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact our office located in North Canton, Ohio . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ingrown Toenails
Ingrown toenails (onychocryptosis) are a common foot ailment and it is very unpleasant to experience. The condition is caused by an increase in pressure from the ingrowth of the nail edge into the skin of the toe. Ingrown toenails commonly cause pain in those who experience them. In some cases, the skin surrounding the ingrown toenail may break which may lead bacteria to enter through and cause an infection. Common symptoms of this ailment include pain, redness, swelling, and warmth around the toe.
An imbalance between the size of the nail and the enlargement of the nail skin edge causes ingrown toenails. This condition is often caused by improperly trimming the toenails. If you are trying you cut your nails, you should always try to trim straight across instead of in a rounded shape. Ingrown toenails can also be an inherited condition and they may also be caused by improper shoe fitting.
Another common cause of the condition is wearing shoes that are either too small or too large. Other causes include poor foot hygiene, obesity, diabetes, arthritis, edema, and fungal infections. There are many risk factors that may make a person more likely to develop an ingrown toenail. Athletes who play “stop and start” sports such as tennis, soccer, and basketball are most likely to have ingrown toenails.
People who have diabetes, a compromised immune system, or poor circulation should immediately seek care from a podiatrist if they have an ingrown toenail. It is also recommended to seek professional assistance if at-home remedies are not successful within a week or if there is persistent pain.
Facts About Rheumatoid Arthritis in the Feet
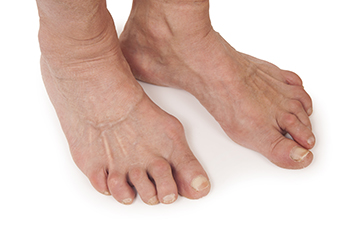
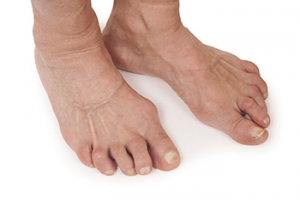
Rheumatoid arthritis, or RA, is an autoimmune disease that affects joints throughout the body including the feet. In RA, the immune system attacks the lining of the joints causing inflammation, pain, and swelling. In the feet, RA typically affects the toes, midfoot, and ankles, often leading to deformities such as hammer toes or bunions. Over time, the cartilage in the joints can wear down resulting in limited mobility and increased pain. People with RA may also experience stiffness, especially in the morning, and difficulty walking or standing for long periods. The inflammation in the feet can worsen with activity making it challenging to wear shoes comfortably. Early diagnosis and treatment are vital in managing symptoms and preventing further damage. Treatment options may include medications and surgery to improve foot function and quality of life. If you have this condition, it is suggested that you confer with a podiatrist who can help you manage RA.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Priyanka Mude, DPM of North Canton Podiatry. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in North Canton, Ohio . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Rheumatoid Arthritis in the Feet
Rheumatoid Arthritis is a chronic progressive disease that attacks several joints throughout the body. It is an autoimmune disease in which the body’s immune system mistakenly attacks the joints. As a result, the tissue inside the joints, called synovium, starts to thicken and causes pain around the joints. The synovium is responsible for creating a fluid that lubricates the joints to help them move. Approximately 1.5 million people in the United States have Rheumatoid Arthritis. Women are almost three times as likely to have RA compared to men, and it’s disease usually begins between the ages of 30 and 60. People who have a genetic history of RA are more likely to develop the disease.
Symptoms of RA may include the following sensations in the joints: pain, tenderness, swelling, redness, warmth, stiffness, and loss of range. Swollen joints are a very common symptom for those with the disease. At times, it may be minimal, but it may also be very apparent. Another typical symptom is joint stiffness. Doctors will often use the direction of morning stiffness to measure the severity of a patient’s joint inflammation. Other RA symptoms include limping, anemia, fever, and fatigue.
To diagnose RA, your podiatrist will typically request x-rays to see how much damage there is in the joints. Blood tests may also be performed to show if there are any signs of anemia, or antibodies such as the rheumatoid factor. If you have previously been diagnosed with RA, you should know the disease may spread to your feet and ankles.
There are many non-surgical options that can be used to treat this ailment. Some of these options include physical therapy, foot massages, orthotics, bracing, supportive shoes, and steroid injections. Physical therapy is useful because it will help stretch and strengthen the joints in both the foot and ankle to improve joint function. Massages can help improve blood circulation which will be good for the feet. Choosing proper footwear will allow you to walk with comfortability if you are a sufferer from RA. Lastly, bracing will help stabilize the foot joints, limit deformities and decrease pain.
In severe cases, surgery may be a treatment option that should be considered. For those who cannot walk without experiencing pain and those whose deformities can not be managed with braces, surgery should be considered. Your podiatrist will recommend surgery if he or she believes it will improve your foot biomechanics.
Vascular Testing by Podiatrists
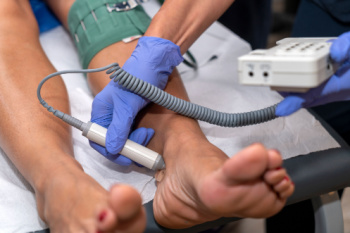
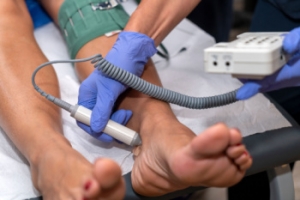
Podiatrists perform vascular testing to assess blood flow in the feet and legs, vital for diagnosing and managing conditions that impact circulation. These tests are particularly important for individuals with diabetes, peripheral artery disease, abbreviated PAD, or chronic foot wounds, as poor circulation can hinder healing and lead to severe complications. Common vascular tests include the ankle-brachial index, or ABI, which compares blood pressure in the ankle to the arm, and Doppler ultrasound, which visualizes blood flow in arteries and veins. Vascular testing helps identify narrowed or blocked vessels, allowing podiatrists to develop targeted treatment plans. Early detection of vascular issues is essential in preventing serious outcomes, including ulcers and, in extreme cases, amputation. If you have cold feet, numbness, or non-healing wounds on your feet, it is suggested that you contact a podiatrist for this kind of testing.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with Priyanka Mude, DPM from North Canton Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
- Ankle-Brachial Index (ABI) examination
- Doppler examination
- Pedal pulses
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact our office located in North Canton, Ohio . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Vascular Testing in Podiatry
In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.
How Wearing High Heels Affects Physique and Gait

Wearing high heels can significantly impact both physique and gait. The elevated heel forces the body to shift its weight forward, which can alter posture and lead to an unnatural spinal curve. This change in alignment often results in tension in the lower back, hips, and knees. Over time, consistent use of high heels can contribute to muscle imbalances, as certain muscle groups, such as the calves, become shortened while others, like the hamstrings, may weaken. Gait is also affected, as high heels cause the wearer to take shorter, less stable steps, increasing the risk of stumbling or twisting an ankle. Additionally, the pressure placed on the toes can lead to foot problems like bunions or hammertoes. If you have developed foot pain from wearing high heels, it is suggested that you consult a podiatrist who can offer relief and treatment tips, in addition to guiding you toward appropriate high-heel choices.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact Priyanka Mude, DPM from North Canton Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
- Ankle Joints
- Achilles Tendon – May shorten and stiffen with prolonged wear
- Balls of the Feet
- Knees – Heels cause the knees to bend constantly, creating stress on them
- Back – They decrease the spine’s ability to absorb shock, which may lead to back pain. The vertebrae of the lower back may compress.
What Kinds of Foot Problems Can Develop from Wearing High Heels?
- Corns
- Calluses
- Hammertoe
- Bunions
- Morton’s Neuroma
- Plantar Fasciitis
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact our office located in North Canton, Ohio . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Effect of High Heels on the Feet
High heels are uncomfortable, but many women sacrifice comfort to be stylish. There are many problems that stem from wearing high heels, however these issues can be avoided by wearing proper shoes.
Heels are bad because they push your weight forward toward the fall of the foot. The higher the heel is, the more weight and pressure get shifted. This process causes the back to hyperextend backwards to counterbalance which may cause pain in the leg, hip, and back. Consequently, major posture problems may occur, and these issues may eventually become permanent.
Wearing high heels is one of the leading cause of ingrown toenails. Heels create a great deal of pressure on the big toenails which disrupts proper toenail growth. This may eventually lead to the big toenail growing into the skin. Another common problem that stems from high heels is bunions. If bunions go untreated, they can cause serious scar tissue to form along with severe pain.
However, there are ways to minimize the harmful risks associated with wearing heels. You should try to massage and stretch your legs and feet after wearing heels for an extended time. Stretching helps prevent the Achilles tendons and calf muscles from becoming too tight. A good substitute for heels are platforms which provide a better surface area to evenly distribute the body’s weight.
If you are experiencing any painful foot conditions from wearing high heels, you should consult with your podiatrist right away.
Let the Expert Treat Your Ingrown Toenails
Ankle Sprains and Anatomy

An ankle sprain occurs when the ligaments surrounding the ankle joint are overstretched or torn, resulting in pain and swelling. The ankle is made up of three bones which are the tibia, fibula, and talus, and held together by ligaments that provide stability. The most common ligaments involved in an ankle sprain are the anterior talofibular ligament and the calcaneofibular ligament. These ligaments help stabilize the ankle during movement. An ankle sprain typically happens when the foot twists or rolls in an unnatural direction, often during activities like running, jumping, or sports. Causes can include walking or running on uneven surfaces, sudden changes in direction, or wearing improper footwear. Symptoms include pain, swelling, bruising, and difficulty moving the foot or bearing weight. If you have sprained your ankle, it is suggested that you promptly schedule an appointment with a podiatrist who can provide an accurate diagnosis and effective treatment.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact Priyanka Mude, DPM from North Canton Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
- Mild to moderate bruising
- Limited mobility
- Swelling
- Discoloration of the skin (depending on severity)
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact our office located in North Canton, Ohio . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.